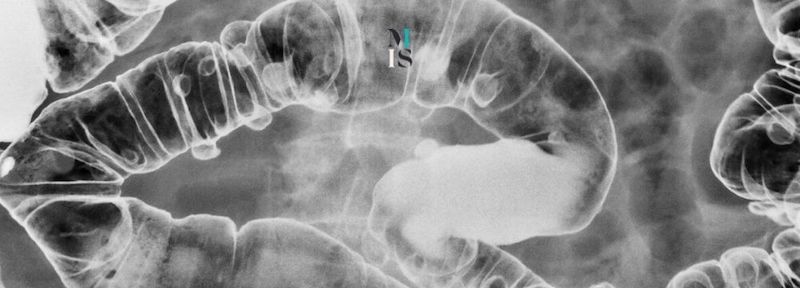
Colon & Rectal
Crohn’s disease is an autoimmune disorder that causes chronic colon or gastrointestinal tract inflammation. Unfortunately, Crohn’s disease has no cure, and while it can go into remission at various times, there is currently no definitive cure.
Humira is a heavily marketed prescription drug for moderate to severe Crohn’s disease patients who have not seen relief with other medication or lifestyle interventions.
Is Humira a Good Choice for Crohn’s Disease?
Humira may be an appropriate option for some patients that haven’t seen results from other medications and are not ready to consider surgical intervention. If Humira seems to work well and the patient goes into remission without unacceptable side effects, it can be continued.
However, we must look at other options if symptoms are not relieved or if the side effects of the drug are severe enough that the patient must stop taking it. While many patients will see good results within four weeks, we use 12 weeks as the benchmark in deciding if the treatment has been successful.
Ultimately, the best philosophy is taking a stepped approach toward care. This means exhausting reasonable lifestyle and medical options before surgery.
What Are the Risks and Side Effects?
Typical side effects of Humira include a reaction at the injection site, which is common with just about any injected drug. Other patients may experience sinus infections, headaches, rashes, and nausea. Individual results will, of course, vary. Be mindful that Humira is an immunosuppressant, and taking it will increase the risk of adverse outcomes if you contract an infection or cancer. This is particularly important during the COVID-19 pandemic.
In the past, many patients inaccurately believed that there was not much that could be done if medication and time did not resolve their Crohn’s disease. However, medication may not always control Crohn’s disease, and patients may be candidates for surgery because of the complications associated with chronic inflammation of the intestine. As the walls of the intestines start to thicken or develop scar tissue, a partial blockage of the intestine known as a stricture can occur. Other issues can include bleeding, perforation of the bowel, fistula formation, abscess formation, and more.
As a result of these potential outcomes and the issues they may cause, surgery is often an appropriate next step to retain as much healthy bowel as possible.
Of course, the first step is to discuss surgery as an option with your primary care physician and general surgeon. We encourage you to schedule a consultation with our office to learn more about your Crohn’s treatment options.