Conversations with Your Doctor
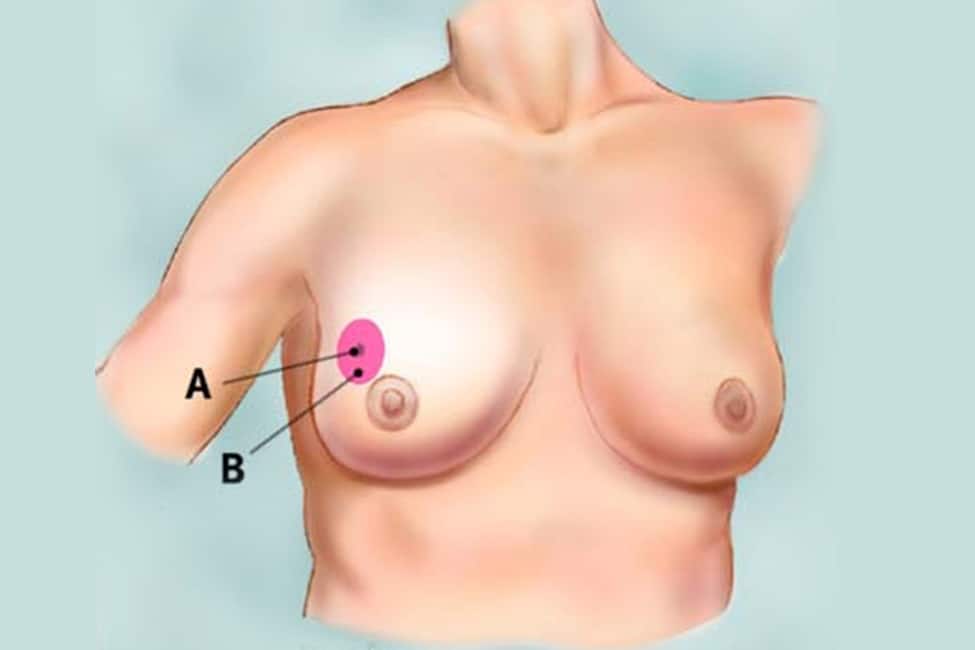
We may recommend lumpectomy if a biopsy has shown that you have cancer and that the cancer is believed to be small and early stage. Lumpectomy may also be used to remove certain noncancerous or precancerous breast abnormalities.
If you and doctor decide lumpectomy is right for you, you’ll meet with them a few days before your lumpectomy. Bring a list of questions to remind you to cover everything you want to know. Make sure you understand the procedure and its risks.
You’ll be given instructions about presurgical restrictions and other things you need to know. In most cases, the surgery will be done as an outpatient procedure, so you can go home the same day.
Tell your doctor about any medications, vitamins or supplements you’re taking in case something could interfere with the surgery. In general, to prepare for your lumpectomy, it’s recommended that you: